April 24th, 2013
Why do I use the "advanced" technology that I do?
I'll be the first to admit that I'm a bit of a tech-geek. I like gadgets and gizmos. Always have. But in medicine, the patient comes first. Medicine, especially surgery, is about balancing the risks of a particular procedure with the proposed benefits. That is certainly true anytime you are considering a technique that hasn't been performed before or applying existing technology in a new way. I council all my migraineurs in this regard when discussing nerve decompression or arterial ligation as a treatment for migraine headaches.
The use of an endoscope - a long, slender camera that can be introduced through half-inch long incisions - in plastic surgery has been around for over a decade. Some applications strike me as silly (using it for a tummy tuck, for example, when you need the incision to remove extra skin). The endoscope is a great tool for brow lifts or for nerve decompression for migraine, as it saves the patient an incision on their upper eyelid or a long incision from ear to ear which can be prone to scarring and hair loss. The use of the endoscope in both facial plastic surgery and various ENT procedures has become relatively routine, as it allows us to view things that are difficult to see through small incisions made some distance from where you're operating (which is vital in the face, where we try to hide or avoid incisions at all costs - for obvious reasons). I have found, though, that another of my preferred uses of the endoscope is repairing jaw fractures that are traditionally left to heal on their own or with a short course of braces and rubber band treatment. Very few surgeons utilize this technique, which is applying existing technology to improve patient outcomes.
Jaw fractures that are near the TMJ are difficult to access because of their location. Located directly in front of the ear, there is lots of "high-price real estate" between the skin and that part of the jaw. Most notably, the facial nerve - the nerve that controls the muscles of the face - lives in this area. Damaging that nerve in front of the ear paralyzes the entire side of the face - an understandably devastating complication for both patient and surgeon. For that reason, few surgeons repair injuries of this part of the jaw, and rather allow it to heal, even though the healing process is imprecise and often leaves patients with abnormalities of their bite.
The use of the endoscope here allows me to repair these injuries with minimal risk to the facial nerve. I introduce a camera through a small incision in the mouth, and the only incisions that are in the skin at all are no bigger than the end of an ink pen and are used to place screws to hold the metal plate in place. Most of the work is done through the mouth. Sure, it takes more time than putting "braces" and rubber bands on, which takes about 20 minutes. This surgery takes about an hour (give or take), which is just a little longer than it takes to make the traditional incision, but without risk to the facial nerve.
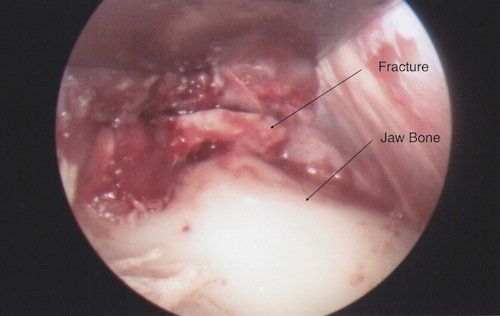
The pictures here tell the story. The first picture is the fracture itself. The second shows the metal plate in place (with what looks to be a giant screwdriver coming down through the cheek), and the final shows the repair just before the procedure ended. Keep the scale in mind - the screws themselves have a diameter of 2 millimeters and the plate is no more than an inch long- so this stuff is pretty small.
Not to be too long-winded, but the purpose of this post is this: new technology is great, the treatment has to fit the problem. Slightly added operating time and expense to prevent a paralyzed face? Sounds like a good trade-off to me. Adding 3 or more hours in surgery and the cost of a million-dollar-plus robot to prevent a well-hidden, 6-8 inch incision for a breast reconstruction? Doesn't make much sense to me.
As my grandmother used to say: "Sometimes the juice just ain't worth the squeeze."
KNOXVILLE, TN
Contact us today to schedule your appointment with renowned plastic surgeon and face, body & breast specialist Dr. Jason Hall. Take your first steps to a more confident and natural you.
9239 Park W Blvd #202, Knoxville, TN 37923